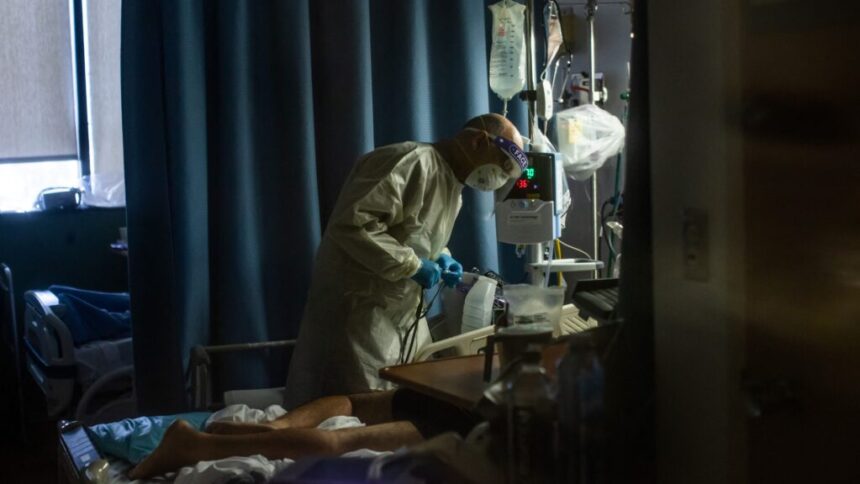
In 2009, I was practicing in the emergency department when the H1N1 pandemic emerged. Then, I saw firsthand the vital role infectious disease physicians played in not only facilitating a coordinated public health response, but also helping patients, providers, and the public navigate the uncertainty that comes with confronting a novel virus. While on the frontlines of that pandemic, I depended on our community’s infectious disease specialists as I worked in real-time to provide patients with the answers and care they needed.
Ten years later, when an even deadlier novel virus swept the country, I encountered that same uncertainty navigating a novel public health threat — this time representing the same communities I once served as a physician. And when Covid-19 struck, the vulnerabilities in our nation’s health care system were laid bare for the world to see. By the end of 2020, more than 350,000 Americans had died of Covid, and health care workers were pushed to the brink. Since then, we have been able to close the door on the worst of these challenging times with the help of investments in public health infrastructure through the American Rescue Plan.
These investments mobilized the largest vaccination campaign in U.S. history, expanded access to testing and treatment for millions of Americans, and bolstered community-based disease surveillance across the country. And while we have made great strides in overcoming Covid in large part because of these efforts, the work to prepare for the next public health emergency remains unfinished.
As an emergency medicine physician, public health expert, and ranking member of the Select Subcommittee on the Coronavirus Pandemic, I am committed to addressing the vulnerabilities in our health care system that continue to haunt us from the earliest days of the pandemic. Among the most glaring of those weaknesses is a depleted public health workforce tasked with not only addressing current threats to the public’s health but also working in real time to prepare us for future threats every day. Central to this work are our nation’s infectious disease physicians, who serve on the front lines when new viruses emerge — promoting our understanding of the risk they pose, treating patients, and guiding infection-control strategies across the country.
Since the days when I fought H1N1 alongside infectious disease doctors, we have seen a startling decline in their ranks. In fact, in the years headed into the Covid-19 pandemic, 80% of U.S. counties lacked an infectious disease specialist according to a study analyzing 2017 Medicare Provider Utilization and Payment Data. Most concerningly, the Health Resources and Services Administration projects that by 2025, the United States will have fewer than 14,000 infectious disease physicians practicing, falling well short of the more than the 15,700 specialists needed to adequately serve our communities. This shortage, the administration says, will likely continue for the next decade. In fact, only about half of infectious disease training programs were filled in 2021, and the number of applicants for infectious disease fellowships dropped in 2023 from 2022.
Infectious disease experts are the cornerstone of a strong, coordinated public health workforce. To reduce harm and save lives in the future, we need to ensure that we have the public health infrastructure in place now that can quickly identify and respond to emerging threats. Without enough infectious disease experts leading this charge, our efforts will surely fall short.
To start, we must remove barriers that hinder aspiring medical providers from pursuing careers in this field. Infectious disease specialists are among the lowest paid in the medical field — earning far less than what many other specialties do despite years of additional training. This may serve as a major barrier for medical students and residents interested in pursuing careers in this field.
We can level the playing field for these specialists while bolstering our nation’s pandemic preparedness with a few simple solutions. For example, Congress and the Centers for Medicare and Medicaid Services can work together to modify the physician fee schedule so that infectious disease physicians can be reimbursed for the additional services they take on as part of their work coordinating responses to outbreaks, such as developing clinical guidelines and standing up testing and vaccination efforts.
Another avenue to encourage the recruitment and retention of infectious disease specialists is to ease the financial burden associated with the additional medical training that those pursuing careers in this specialty must complete. For example, policymakers can comprehensively invest in the Public Health Workforce Loan Repayment Program and the Bio-Preparedness Workforce Pilot Program. Last year, Congress established these programs in the Consolidated Appropriations Act of 2023 as part of larger efforts to strengthen the country’s overall pandemic preparedness. By investing in these programs in upcoming appropriations packages for fiscal year 2025, we can provide targeted loan repayment to infectious disease clinicians who work in areas that are underserved or experiencing acute health professional shortages.
By taking such steps, we will not only improve patient outcomes today, but we will also grow a robust, prepared workforce ready when — not if — the next pandemic strikes.
Rep. Raul Ruiz, M.D. (D-Calif.), is the ranking member of the House Select Subcommittee on the Coronavirus Pandemic. He is an emergency medicine physician and serves on the House Energy and Commerce Committee. He is in his sixth term.